
IUD Pros and Cons
By Kimberly Kushner
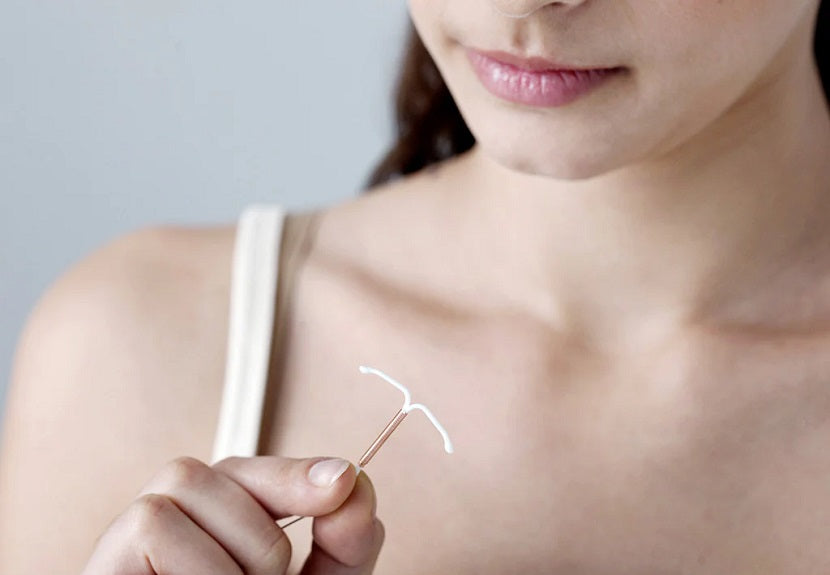
Some women love their hormonal IUD, whilst others haven’t had the best experience with theirs. Although this may be a controversial topic, the intention of this article is to simply explain the potential safety issues of a hormonal IUD so that you can then make better, informed decisions about your health.
How does a hormonal IUD work?
Simply put, a hormonal IUD releases levonorgestrel. Levonorgestrel is a synthetic progesterone that will:
- Thicken cervical mucus, hindering sperm from traveling into the uterus.
- Thin the uterine lining, preventing egg implantation.
- Inhibit sperm movement, preventing sperm from reaching an egg.
These factors combined make the IUD an effective contraceptive device. Its ability to thin the uterine lining also makes it the preferred medical device to aid with heavy and painful periods among many doctors and medical specialists. It is important to note, however, that users may still experience a light bleed because the hormonal IUD does not always shut down ovulation.
While blood levels of levonorgestrel are much lower in women who have an IUD compared to those using the oral contraceptive pill because a hormonal IUD releases levonorgestrel locally, you can still experience side effects from it. To put numbers in perspective, the pill has about 1 milligram of progestin, while an IUD releases about 20 micrograms of progestin daily. This is reduced to 10 micrograms a day after 5 years, and 9 micrograms a day after 6 years.
Side effects of a hormonal IUD
Levonorgestrel is a synthetic progesterone and is very different from the natural progesterone that our bodies make. Natural progesterone is only made as a result of the process of ovulation. It is synthesised by the corpus luteum, which are remnants of the tiny sac that your egg released each time you ovulate.
From a chemical perspective, levonorgestrel is interestingly comparable to testosterone in shape and structure. Because of this, it can result in symptoms similar to what excess testosterone can cause. Commonly experienced ‘androgenic’ side effects of a hormonal IUD include:
- Acne
- Hirsutism (excess facial hair and male hair growth patterns)
- Hair loss
- Depression, anxiety, or mood swings (If you have tried the oral contraceptive pill and experienced severe mood swings whilst you were on it, you will probably experience the same thing with an IUD.)
Other side effects of an IUD include:
- Headaches/migraines
- Excess vaginal discharge and yeast infections
- Vulvovaginitis
- Weight gain
- Breast pain
- Abdominal pain, cramping, and nausea
- Hypersensitivity reactions like rashes or hives
- Irregular bleeding, especially for the first 6 months (You may experience spotting or heavier bleeds.)
- Irregular periods (The Mirena does not completely shut off your menstrual cycle.)
- Absence of bleeding (You may stop getting bleeds altogether and if this does happen, it usually after 1 year of having an IUD.)
Those using an IUD should also look into these other possibilities:
- An IUD can cause ovarian cysts to form. Although these often disappear on their own, sometimes they do not and may require surgical removal.
- An IUD can be expelled by your body. This is most common in younger women.
- Levonorgestrel can pass through breast milk. If you have an IUD and are nursing, the hormone can be passed on to your baby.
- An IUD can cause perforation of the uterus. In rare cases, it can go through the wall of the uterus. This is more likely if you are breastfeeding.
A very small percentage of women who have an IUD can get pelvic inflammatory disease (PID). For this reason, an IUD is not for you if there’s a possibility you have sexually transmitted infections or genital infections. It is also important to note that an IUD does not protect against infections. Additionally, if you have or had breast cancer, then all hormonal contraceptives should be avoided.
Rare but serious adverse reactions have been linked to the IUD and these include:
- Blood clots, deep vein thrombosis and stroke
- Markedly high blood pressure
-
Ectopic pregnancies (A very small percentage has been reported with IUD use and risk is higher if you have a history of an ectopic pregnancy, tubal surgery or pelvic infections.)
- Group A Streptococcal sepsis (Although rare, this has been reported following the insertion of IUDs.)
The IUD and your menstrual cycle
Because an IUD will usually suppress ovulation, this prevents your body from producing its natural sex hormones. As a result, it will inhibit your menstrual cycles.
There are benefits of going through your natural cycles, including the process of your body’s production of estradiol and progesterone. When using or taking anything that suppresses your cycle, you do not get the protective benefits of your endogenous hormones.
For women, natural, healthy levels of both estrogen and progesterone have health benefits which include:
- Cardiovascular benefits (estrogen and progesterone are cardioprotective)
- Connective tissue support (estrogen keeps our skin supple while progesterone can help prevent hair loss)
- Musculoskeletal support (estrogen can prevent osteoporosis)
- Mood, sleep, anxiety (progesterone aids with GABA production, an inhibitory brain chemical)
- Balances androgens, which are male sex hormones (progesterone can be anti-androgenic but progestins are androgenic)
The naturopathic approach
From a naturopathic perspective, we see great value in going through your natural cycles and having regular periods. This is because your period is like your monthly hormonal report card, which gives good insight into what’s going on inside your body.
Details such as the length of your bleed, the presence or absence of pain, the nature of your flow, and various other symptoms you may be experiencing through your menstrual cycle are all very important in determining if you should opt for an IUD in the first place. These are the various factors that we aim to address naturopathically in order to achieve optimal hormone balance. We want to encourage you to avoid suppressing symptoms by band-aiding a condition or addressing imbalances with synthetic hormones.
Providing your body with an external source of synthetic progestins can result in your brain interpreting this as your body having plenty of natural progesterone, when in fact it doesn’t. Because your body thinks that it has enough, this can then switch off your natural progesterone production. This can have further implications on your hypothalamic-pituitary-ovarian (HPO) axis, which is the communication line between your brain and ovaries that is involved in the manufacture of sex hormones.
One of the potential issues this may cause is high levels of unopposed estrogen or estrogen dominance due to lower levels of natural progesterone. Often, women get an IUD fitted for symptoms of oestrogen dominance to begin with. These symptoms include heavy, menstrual bleeds and menstrual pain. So as you can see, the IUD does not address the underlying root cause; instead, it simply band-aids the symptoms. You can read more about symptoms of oestrogen dominance and the naturopathic approach to addressing it here.
Hormone metabolism and oestrogen dominance
The levonorgestrel contained in IUDs is metabolised via a group of liver enzymes called the “CYP 450” enzymes– specifically, the CYP3A4 enzyme pathway. This specific enzymatic pathway is responsible for the metabolism and detoxification of our body’s oestrogen. Interestingly, both levonorgestrel and oestrogen (E1 or estrone, specifically) share the same detoxification pathway and undergo metabolism via this CYP3A4 enzyme.
The CYP3A4 enzyme metabolises Estrone (E1) – one of your three types of oestrogen – and creates 16-OH-E1, the most estrogenic of all the oestrogen metabolites. If you are already dealing with symptoms of oestrogen dominance and excess production of 16-OH-E1, placing an additional burden on your detoxification system by giving it levonorgestrel to detoxify can further perpetuate your underlying oestrogen dominance symptoms.
Summary
The IUD can be an alternative method of contraception for women who cannot take the pill, but it does not come without potential adverse reactions and side effects. It is important to understand that an IUD may also mask or band-aid potential underlying hormonal imbalances.
REFERENCES
Dal'Ava N, Bahamondes L, Bahamondes MV, Santos AO, Monteiro I.(2012). Body weight and composition in users of levonorgestrel-releasing intrauterine system. Contraception Oct;86(4):350-3.
https://doi.org/10.1016/j.contraception.2012.01.017
Jatlaoui TC, Riley HEM, Curtis KM. (2017), The safety of intrauterine devices among young women: a systematic review. Contraception. Jan; 95(1): 17–39.
https://dx.doi.org/10.1016%2Fj.contraception.2016.10.006
Wu JP, Pickle S. (2014), Extended use of the intrauterine device: a literature review and recommendations for clinical practice. Contraception. Jun; 89(6):495-503.
https://doi.org/10.1016/j.contraception.2014.02.011






Leave a comment
This site is protected by hCaptcha and the hCaptcha Privacy Policy and Terms of Service apply.