
Natural Menopause Management Plan
By Jeff Butterworth
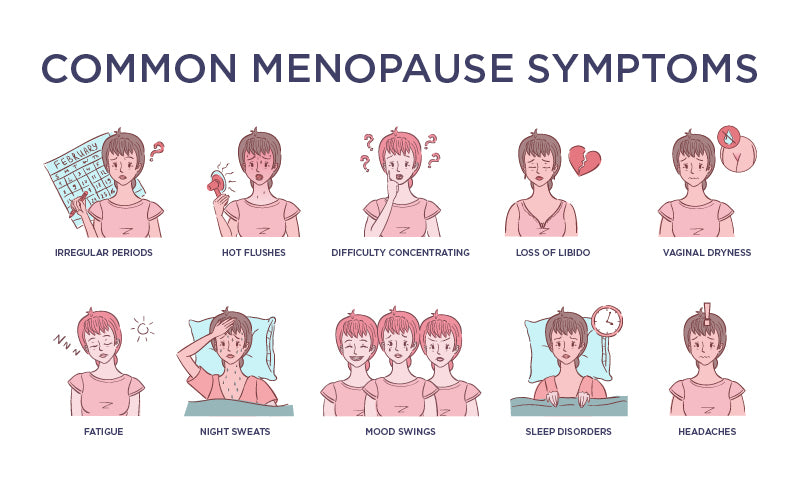
Menopause can be a difficult phase in life. Symptoms of hot flashes, sleeplessness, weight gain, irritability, aches and pains, itching skin, and reduced libido are a few of the challenges women have to face.
You certainly are not alone - with 85% of women reporting symptoms associated with menopause. Menopause is a natural process, and yet it is treated as a disease… hence women struggle to find effective treatments.
"The secret to managing menopause effectively in the short and long term is to
support the body through its natural process."
What is the Natural Process of Menopause?
As women approach menopause, their natural production of progesterone and oestrogen from the ovaries reduces. A little known fact but a VERY important one is that the body shifts its hormone production from the ovaries to other areas of the body - primarily the adrenal glands, breast tissue, fat cells and even the brain.
The misconception is that menopausal and postmenopausal women produce very small amounts of oestrogen and zero progesterone. This is true, however, the body changes the forms of hormones produced. Estrodiol E2 drops, however Estrone E1 becomes the dominant form of oestrogen and the body becomes dependent on androgen conversion from the adrenals for hormone levels. Interestingly Chinese and Japanese women had the highest levels of a hormone called DHEAS during and post menopause.
This is very important to understand as the successful transition through menopause depends on stimulating the body’s own production of hormones, rather than providing external hormones, which effectively prolongs the menopausal process.
Average age of menopause
The average age women enter menopause is 49 to 51 and is officially classified as one year without a menstrual cycle. This classification is erroneous, however, as the process of perimenopause and eventually menopause begins up to 5 years prior as cycles become erratic. Symptoms of menopause can begin well before the cessation of a cycle, with some women waiting to be officially diagnosed with menopause before seeking help.
The mistake here, again is putting a disease label on a natural process. It is a process and part of a woman’s reproductive journey. Support the process and women are able to successfully navigate this time of life and flourish.
Menopause is not a disease
Menopause is going to happen… it is inevitable and a fact of life. Classifying menopause as a disease is not only the wrong approach long term, but it creates a stigmatism for women that can impact in many areas of their personal, work and social lives.

How to Manage Menopause Naturally
Menopause is NOT a disease and the successful navigation of menopause depends on supporting your body, not suppressing symptoms. Symptoms can be avoided and minimised when the body is given the right tools and environment to flourish because every woman will have their own unique experience with menopause. The best approach is a holistic one, and I will outline at the end of this article the generalised approach to managing menopause. First, let’s look at the most challenging symptoms associated with menopause, why they occur, and tips to minimise them.
Sleep
The most commonly reported symptom women suffer are sleep disturbances. Poor sleep is also a compounding factor for all the other symptoms associated with menopause. It is often assumed that poor sleep during menopause is associated with the symptoms of menopause such as hot flashes. This is true, however, a deeper endocrine imbalance is at fault. The production of natural melatonin reduces during menopause. Melatonin is your body’s natural sleep hormone and reduced levels of melatonin during menopause in combination with disruptive sleep symptoms such as hot flushes is the reason why many women suffer from poor sleep.
A positive approach to improving sleep during menopause is to encourage the production of natural melatonin and, of course, manage hot flashes in particular. There are also many other tips to improving sleep quality and stimulating natural melatonin which can be investigated in this article.
Stress
Stress is one of the major factors in triggering hot flushes. During episodes of stress the release of epinephrine (also known as adrenaline) from the adrenal glands causes the heart to beat faster and blood flow to increase. Stress also places a long-term strain on the adrenal glands which should be focusing on hormone production during the menopausal transition. Stress is accumulative, so it is important that you implement regular stress-release techniques. Exercise, yoga, meditation, reading a book and even time management techniques should all be part of a regular focus on reducing and managing stress during menopause.
Weight gain
Weight gain is a constant complaint from our community of women going through menopause, and there is a physiological reason why. Diet of course plays a pivotal role, however, it is important to understand why women gain weight when they start to enter menopause.
Earlier in the article I discussed how the body shifts its hormone production from the ovaries to the adrenals, breast and fat cells. FAT CELLS!! Yes… there is a metabolic reason why you are gaining weight. Your body is hoarding fat to assist with the production of your hormones which are needed for your overall wellbeing.
BUT… there is a hack. By stimulating the adrenals to produce the necessary hormones needed during menopause, your body will be less reliant on fat cells. Less reliant, but there is no way of totally short-circuiting nature. This metabolic phenomenon will always exist, so our approach is to use healthy meal replacements for one meal a day to reduce your overall calorie intake.
Another interesting fact is that exercise reduces the severity and frequency of hot flushes. Several studies show that regular, moderate exercise reduces hot flushes by improving the thermodynamic control of the body. Exercise also assists with elevating feel-good hormones and reducing depression and anxiety.
Bladder issues
Urinary symptoms are common as women age, which are related to a reduction in hormone levels, as well as structural issues developed from childbirth, operations, prolapses and changes in mycology.
A weakened bladder can be the cause of many embarrassing and uncomfortable symptoms during menopause and beyond. 50% of women over the age of 50 experience some form of bladder weakness and incontinence. A weak bladder also contributes to poor sleep with women having to urinate several times during the night. Aside from Kegel exercises, there are natural herbal medicines which can tone the bladder and improve symptoms.
Hot flashes
The most dramatic symptom which usually forces women to seek treatment is undoubtedly hot flashes. The severity and duration of hot flushes vary from woman to woman, yet the same mechanism remains in place. The drop and fluctuations in oestrogen are primarily to blame, and stimulating your body to produce its own levels of hormones is the secret to successfully navigating menopause and managing hot flushes.
Thankfully, nature has provided us with the tools to stimulate the body to do exactly that. Herbal medicines can assist the body to manage the symptoms of menopause. The most common adaptogenic herbal medicines to do this are sage, vitex, black cohosh, and maca. All of these herbs have been specifically included in therapeutic dosages in Happy Hormones.
Hair loss and facial hair
As hormone levels drop, and the body starts to utilise androgens more as a primary source of hormones, hair thinning, and facial hair can become an issue for some women. Three natural medicines can be used to encourage the healthy conversion of these androgens. Kelp, zinc, and silica all work to prevent hair loss and facial hair from developing.

Dietary and lifestyle factors
The more balanced your internal body biochemistry, the better your chance of avoiding the main symptoms associated with menopause.
Common dietary triggers of hot flashes:
Treatment Guidelines Summary
Natural medicines can be used as tools to accelerate the transitional process and encourage the body to produce the necessary levels of hormones it needs for its wellbeing, and to avoid many of the symptoms commonly associated with menopause.
- Consume a plant-based diet, avoiding sugar, alcohol, and caffeine specifically.
- Exercise regularly to reduce hot flashes and improve mood and sleep.
- Focus on a healthy sleep routine.
- Implement stress management/release techniques regularly
- Use natural medicines wisely to support your body to transition and produce its own hormone production.
Our protocol is used successfully by thousands of women to manage their menopausal process. If you need additional guidance and support, our practitioner team are available for advice - and even offer online consultations to develop your own bespoke management guideline.

References
Bailey TG, Cable NT, Aziz N, Dobson R, Sprung VS, Low DA, Jones H. Exercise training reduces the frequency of menopausal hot flushes by improving thermoregulatory control. Menopause. 2016 Jul;23(7):708-18. doi: 10.1097/GME.0000000000000625. PMID: 27163520.
P. Kenealy, A. Kapoor, K. A. Guerriero, K. L. Keen, J. P. Garcia, J. R. Kurian, T. E. Ziegler, E. Terasawa. Neuroestradiol in the Hypothalamus Contributes to the Regulation of Gonadotropin Releasing Hormone Release. Journal of Neuroscience, 2013; 33 (49): 19051 DOI: 10.1523/JNEUROSCI.3878-13.2013
Toffol E, Kalleinen N, Haukka J, Vakkuri O, Partonen T, Polo-Kantola P. Melatonin in perimenopausal and postmenopausal women: associations with mood, sleep, climacteric symptoms, and quality of life. Menopause. 2014;21(5):493–500. [PubMed] [Google Scholar]
Vakkuri O, Kivelä A, Leppäluoto J, Valtonen M, Kauppila A. Decrease in melatonin precedes follicle-stimulating hormone increase during perimenopause. Eur J Endocrinol. 1996;135(2):188–192. [PubMed] [Google Scholar]








Leave a comment
This site is protected by hCaptcha and the hCaptcha Privacy Policy and Terms of Service apply.